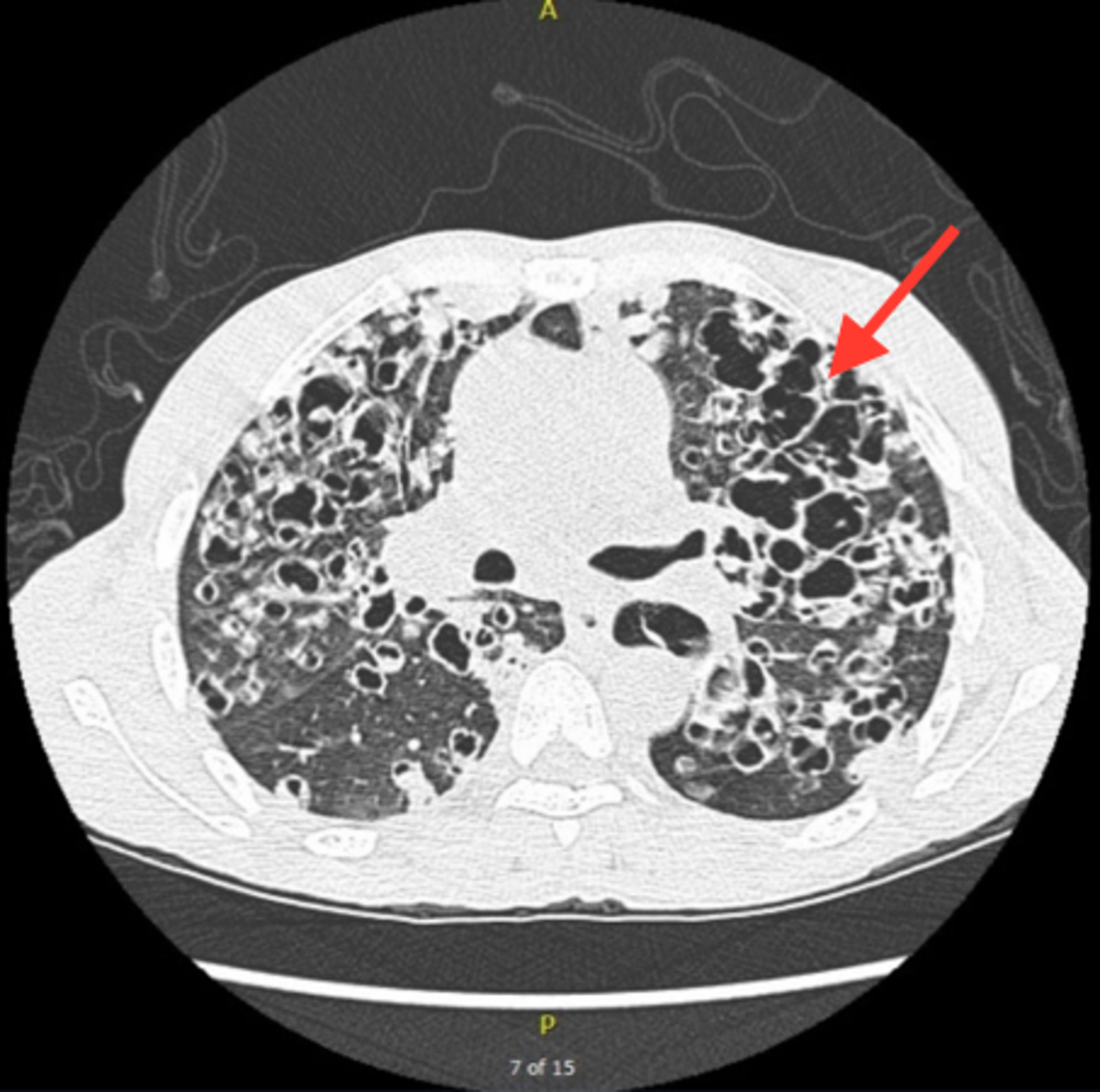
Case ReportĪ 12-year-old Caucasian girl was diagnosed with gastric and ileocolonic Crohn’s disease (CD), Paris classification 元, L4a, B1, G1, having presented with growth failure and abdominal pain and having undergone endoscopic and magnetic resonance enterography assessment. jirovecii) infection requiring intensive care in a pediatric patient with IBD. We present the first case of severe Pneumocystis jirovecii (P. We report a case that highlights the importance of considering opportunistic infection in immunosuppressed pediatric patients with inflammatory bowel disease (IBD) who present with unusual symptoms. Immunosuppressive therapy is a known risk factor for opportunistic infections ( 1). Although there is no place for global PCP prophylaxis in IBD given the low incidence, in an era when there is increasing use of biologic agents with combination immunosuppressive therapy, the risk-benefit profile of PCP chemoprophylaxis should be revisited in selected cohorts such as patients on triple immunosuppression with corticosteroids, thiopurines, and a biological agent or calcineurin inhibitor, especially in lymphopenic individuals. Moreover, it should give gastroenterologists the impetus to limit immunosuppressive therapy to its minimal effective dose and consider options such as exclusive enteral nutrition wherever possible. This report highlights the importance of considering PCP in immunosuppressed lymphopenic pediatric IBD patients who present with unusual symptoms. 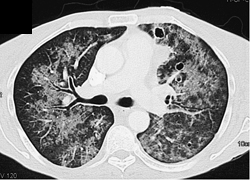
Rates of mono, dual, triple, and quadruple immunosuppression therapy were 35, 35, 29, and 2%, respectively. 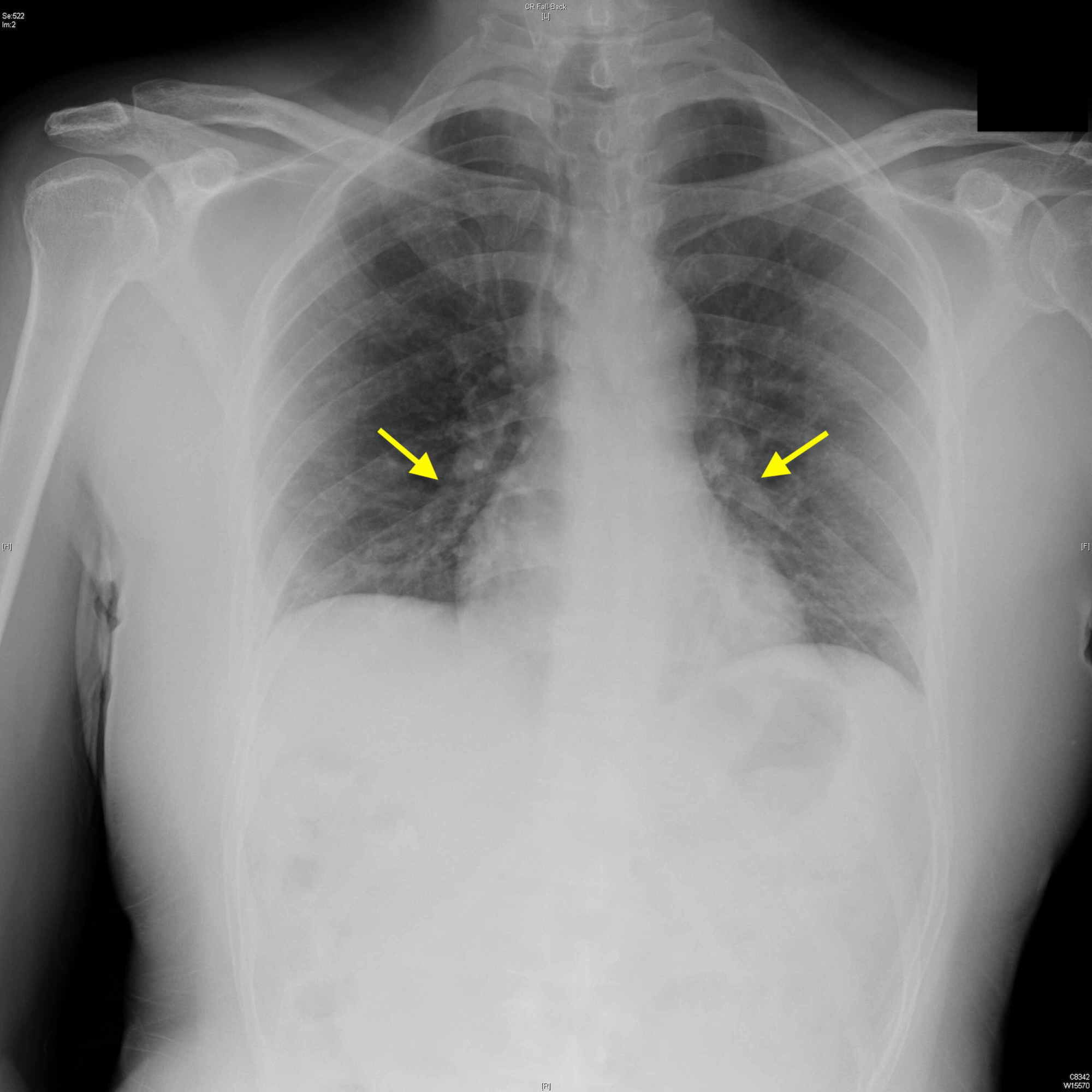
Corticosteroids were used as IBD treatment in 88% of patients who subsequently developed PCP, 42% received thiopurines, 44% used anti-TNF therapy, and 15% received either cyclosporine or tacrolimus. The median age was 45 years (interquartile range 30–68, range 8–78) and 86% of patients were lymphopenic. Overall, 56% of patients were males and 58% had Crohn’s disease. Most sources were case reports and there was likely reporting bias toward patients receiving immunomodulators, anti-tumor necrosis factor (anti-TNF) therapy, and those who died. The literature was reviewed and there were 92 reported cases of Pneumocystis pneumonia (PCP) in patients with IBD. We report the first case of severe Pneumocystis jirovecii infection requiring intensive care in a pediatric patient with inflammatory bowel disease (IBD). Immunosuppressive therapy is a known risk factor for opportunistic infections. 2Vaccine Evaluation Center, BC Children’s Hospital Research Institute, University of British Columbia, Vancouver, BC, Canada.1Department of Pediatric Gastroenterology, Hepatology and Nutrition, BC Children’s Hospital, University of British Columbia, Vancouver, BC, Canada.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
